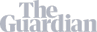Chlamydia and gonorrhea are two of the most commonly reported bacterial sexually transmitted infections (STIs) in the United States [1]. While both STIs are curable with the right treatment, they are often asymptomatic. This can result in delayed diagnoses and increase the risk of serious complications and health consequences.
Infections may also go undiagnosed if sampling is limited to urogenital sites because some individuals only participate in oral and/or anal intercourse. Multi-site screening for these STIs can help increase the likelihood of detecting infections, especially in individuals who may be asymptomatic or have infections located in less commonly tested anatomical sites.
Here’s more about multi-site sexual health testing for chlamydia and gonorrhea and how home sample collection options can improve access to more comprehensive care and reduce the risk of missed infections.
What is chlamydia?
Chlamydia is the most commonly reported STI in the United States, with 1,649,716 reported cases of infection in 2022 [2]. This STI can be contracted during oral, vaginal, or anal sex. It often doesn't cause symptoms, so people may not know that they have it. Only about 25% of women and 50% of men get symptoms, meaning that many of these cases likely go unreported [3]. Antibiotics can treat chlamydia, but without treatment, this STI can cause serious health problems, such as pelvic inflammatory disease (PID), infertility, and an increased risk of human immunodeficiency virus (HIV).
What is gonorrhea?
Gonorrhea is another commonly reported STI in the United States., with a total of 648,056 cases of gonorrhea reported in 2022 [2]. Gonorrhea often has no symptoms. Only about 20% of females and about 10-15% of males will develop symptoms of a gonorrhea infection [4]. Even without symptoms, gonorrhea can cause serious health problems such as infertility, complications in babies, and increased risk of HIV.
Challenges in controlling chlamydia and gonorrhea infections
Earlier detection and treatment are needed to control chlamydia and gonorrhea infections. Yet, a significant challenge is that most STIs are asymptomatic and require testing to identify infection and prevent onward transmission. Home sample collection for STIs can improve access to sexual healthcare across communities and help increase screening and detection.
However, self collect testing options are largely limited to urine and vaginal swabs, limiting the detection of extragenital infections. As a result, there is a need for expanded extragenital bacterial STI testing options.
The importance of multi-site sexual health testing
Urine is commonly used for testing for chlamydia and gonorrhea, but other sites can be affected, like your throat and rectum. These STIs are highly transmissible and often asymptomatic, meaning that early detection relies on regular and comprehensive testing of multiple anatomic sites for those at higher risk.
Multi-site STI screening, or extragenital testing, involves screening different anatomic sites to ensure that an STI is not missed, as it may have been if a patient was screened at only one site.
This comprehensive method is important because different sites may be infected with different organisms. For example, testing genitals only would miss a gonorrhea infection in the throat, which could lead to ineffective treatment.
Studies have shown that extragenital testing (rectal and throat) of chlamydia and gonorrhea increases the detection of infections compared with genital testing alone. One study found that approximately 13% of extragenital gonorrhea infections in an STI clinic would go undetected if tested for genital sites alone [5]. Another study found that up to 33% of gonorrhea diagnoses were missed with urine specimens alone [6].
Who should receive multi-site sexual health testing
The Centers for Disease Control and Prevention (CDC) recommends screening for extragenital infection mainly based on reported sexual activity. Extragenital infections are more commonly reported in women, transgender individuals, and men who have sex with men (MSM) compared with cisgender non-MSM [7].
The CDC recommends annual extragenital chlamydia and gonorrhea screening for MSM, while additional screenings are recommended for women and transgender or gender-diverse individuals if certain sexual behaviors and exposures are reported.
How home sample collection can break down barriers to STI screening
Extragenital infections may also be present among those who both report and deny anal and oral sex. The prevalence of extragenital infections in individuals who deny high-risk sexual behavior may be due in part to avoidance of self-reporting caused by fear of stigma and discrimination. Additionally, the gender nonbinary and transgender community often reports discrimination in healthcare settings, which can lead to avoidance of preventive care services and delayed treatment.
Screening and detection may increase with the availability of home sample collection options that do not require an in-person visit to a healthcare facility. The ability to collect samples from the convenience and privacy of home offers the patient a feeling of safety and anonymity. This can help increase access to STI screening, particularly in hard-to-reach populations that are unable or unwilling to visit a healthcare provider.
About LetsGetChecked’s multi-site sexual health testing solution
There is an imminent need to increase the accessibility of comprehensive STI screening, including detecting extragenital infections. However, many at-home sample collection options are limited to detecting urogenital infections.
LetsGetChecked’s multi-site sexual health screening solution for chlamydia and gonorrhea makes it easy to provide more comprehensive care and reduce the risk of missed infections. This solution includes three components: a urine sample, a throat swab, and a rectal self-swab to maximize the identification of infection at the site of exposure.
Our solution uses at-home sample collection, offering patients a comprehensive and non-stigmatizing approach to sexual health testing without reducing the clinical performance of laboratory testing.
References
- https://www.ncbi.nlm.nih.gov/books/NBK573159/
- https://www.cdc.gov/std/statistics/2022/overview.htm
- https://www.webmd.com/sexual-conditions/most-common-stds-men-women
- https://www.verywellhealth.com/facts-about-gonorrhea-5496694
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10207946/
- https://pubmed.ncbi.nlm.nih.gov/18607315/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10184802/